Uterine Fibroids
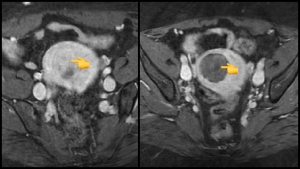
Uterine fibroids are benign growths of the uterine muscle occurring in 30-40% of women. The etiology of fibroids remains the subject of research but genetics is an important factor. The tumors are sensitive mainly to estrogen and progesterone. Most fibroids do not cause any problems and do not require treatment. Some fibroids, however, can cause heavy periods which can lead to anemia and debilitation, or if the fibroids grow large they can lead to ‘compression syndrome’ in which adjacent organs may be compressed such as the bladder leading to frequency of urination, the bowel leading to constipation and bloating. Fibroids may press on nerves causing backache and sciatica and can cause cosmetic unsightliness by bulging the abdomen.
Uterine Fibroid Embolization
Uterine fibroid embolization, or UFE , is performed by interventional radiologists, who consults to evaluate whether UFE is right for the patient. Interventional radiologists are physicians who use X-rays and other imaging techniques to see inside the body and guide tiny catheters and other micro-tools to perform fibroid embolization and treat other conditions without surgery.
Uterine fibroid embolization is not performed by gynecologists, who, for various reasons, may sometimes not discuss it as a possible option for their patients with fibroid tumors. This may occur because gynecologists are not familiar with the procedure or the favorable results of clinical studies. Sometimes they are unaware that UFE is an FDA-approved treatment for fibroid tumors, and may mistakenly tell patients that it is “experimental”. In fact, the procedure has now been recognized by the American College of Obstetrics and Gynecology as a treatment for fibroid tumors. More information is available on the ACOG site.
UFE has several advantages over the other treatments for uterine fibroids.
It involves no blood loss, no stitches or surgical incision (only a small nick in the skin), no abdominal scar, no general anesthesia, no prolonged hospital stay, and no burning or scraping the lining of the uterus.
Uterine fibroid embolization requires much less time off work than hysterectomy (a few days to a week, versus six weeks or more).
One advantage compared to myomectomy is that uterine fibroid embolization can be used to treat all fibroids at the same time, regardless of their size or location in the uterus.
Unlike treatment with Lupron, premature symptoms of menopause are not usually induced. The materials used for uterine fibroid embolization are well tolerated and FDA-approved for embolization.
The cost of UFE varies, but is comparable to or less than the cost of hysterectomy or myomectomy.
Papers on this topic are available at these professional publication sites:
Hysterectomy paper | Myomectomy paper (links to publication sites)
In the few cases that fibroid embolization is not successful and surgery is needed, the operation is typically easier after UFE, with much less bleeding.
How Uterine Fibroid Embolization is Performed
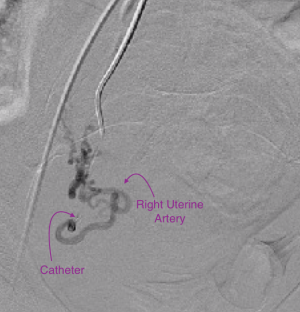
Uterine fibroid embolization blocks, or “embolizes” the blood vessels that “feed” the uterine fibroid, causing it to shrink. The interventional radiologist performs the fibroid embolization through a tiny tube called a catheter which is inserted into an artery at the top of the leg. The patient is given a local anesthetic to numb the skin and a mild sedative, so the procedure is not painful. A special X-ray machine that creates moving pictures in “real” time enables the doctor to see the catheter as it is guided through the blood vessels and into the uterine artery. A contrast agent, or dye, is injected to highlight the blood vessels in the uterus to create an “arteriogram,” an X-ray that maps the arteries feeding the fibroids.
The final step in fibroid embolization is the injection of tiny particles through the catheter. The particles lodge in the blood vessels feeding the fibroids and cut off their blood supply, but the uterus and ovaries are spared. After uterine fibroid embolization, the fibroids begin to shrink. The catheter is removed and the patient is observed overnight, and usually goes home the next day. The fibroids continue to shrink for several months after fibroid embolization.
Who Should Have UFE
Patients who have symptomatic uterine fibroids (abnormal bleeding, pain or other symptoms) may be considered for UFE. Each woman is an individual, and should discuss the potential risks and benefits of UFE and other treatments with her doctors to decide which option is best for her.
UFE and Pregnancy
Women who wish to have children usually are advised to consider myomectomy first, since it is the current recommended therapy. Since UFE also spares the uterus, it may be an option for some. In some cases, the number, size, or position of the fibroids make myomectomy difficult, and increase the likelihood that a hysterectomy will eventually be required. In some patients, fibroids have recurred after myomectomy. For these women, UFE may be a reasonable choice.
The effect of UFE on fertility cannot be predicted in any particular case, and more studies are needed before UFE can be recommended as the first choice for women who desire pregnancy. Nonetheless, many women have reported successful pregnancies after UFE. A small percentage of women experience the onset of menopause after the procedure. This is uncommon in women under the age of 45 but increases as women approach the normal age of menopause. I n one study (.pdf file), 17 pregnancies were reported by women after they had the procedure. Of these, 14 resulted in live births and 3 in miscarriage. One of the women who gave birth to a healthy baby after UFE had suffered 9 miscarriages before she had the procedure.
Postmenopausal women usually are not considered for UFE, since fibroid symptoms tend to lessen or go away after menopause. Recent studies have shown, however, that UFE can be very effective in post-menopausal women.
Success Rates
In approximately 80-90 percent of cases, UFE successfully treats bleeding, pain and other symptoms of fibroids.
The procedure is considered successful if symptoms are gone or greatly improved at three to six months after UFE and no other (surgical) procedure is needed. Abnormal fibroid bleeding usually stops within one to two months, but it may stop immediately. On average, fibroids shrink from approximately 40 percent to 60 percent in six months, and they may continue to shrink for a year or more. Symptomatic improvement may occur independent of the amount of shrinkage.
Avoiding the Risks of Surgery
UFE is an especially good option for women with medical conditions that might increase the risks and complications of surgery. Also, since there is virtually no blood loss or need for transfusions with UFE, it may be ideal for patients who wish to avoid transfusion for health or religious reasons.
Complications and Side Effects of UFE
The low incidence of serious complications that has been reported with Uterine Fibroid Embolization makes this procedure relatively safer than surgery.
Almost all patients have crampy pelvic pain for six to twelve hours after UFE, which is controlled with pain relieving medication. This may be managed with an epidural catheter, or an IV pain medicine pump (PCA). One-third of patients may have a low-grade fever for a week or two, which usually is treated with Ibuprofen. A brief, self-limiting syndrome of high fever and elevated white blood cell count that subsides on its own is experienced by a small percentage of patients. The procedure may cause mild, spotty bleeding for a few months or a brown discharge. Patients are carefully screened for infections before UFE and antibiotics are given during the procedure to decrease the probability of infection. Delayed infections may occur in 3-4 percent of patients, which can be successfully treated with antibiotics in the majority of cases, but occasionally require hysterectomy. There have been reported cases of patients who stopped menstruating temporarily after the procedure, and some patients have gone into menopause, but this is uncommon in women under the age of 45. It is more common in older women who are approaching menopause. Nonetheless, premature menopause must be considered a potential risk.
Damage to other pelvic organs during UFE is extremely rare. This is a potential risk, however, and has been described in pelvic embolization done for other reasons, such as cancer. This is an extremely unlikely occurrence in the hands of a well-trained interventional radiologist.
Although there is some risk associated with all medical procedures, UFE has been shown to be safer and have fewer risks and complications when compared to surgery such as hysterectomy or myomectomy to treat fibroids. If the risk of death from hysterectomy is 1/1000 or 1/1500, the risk of death from UFE might be less than 1/10,000.
The above information is not all inclusive of the risks, alternatives and benefits. It is not meant to be a substitute for informed discussion between you and your doctor, but can act as a starting point for such a discussion. There are complications possible with any medical procedure. Overall, minimally invasive procedures have a lower complication rate than open surgeries.